Welcome to this week’s Research Roundup. These Friday posts aim to inform our readers about the many stories that relate to animal research each week. Do you have an animal research story we should include in next week’s Research Roundup? You can send it to us via our Facebook page or through the contact form on the website.
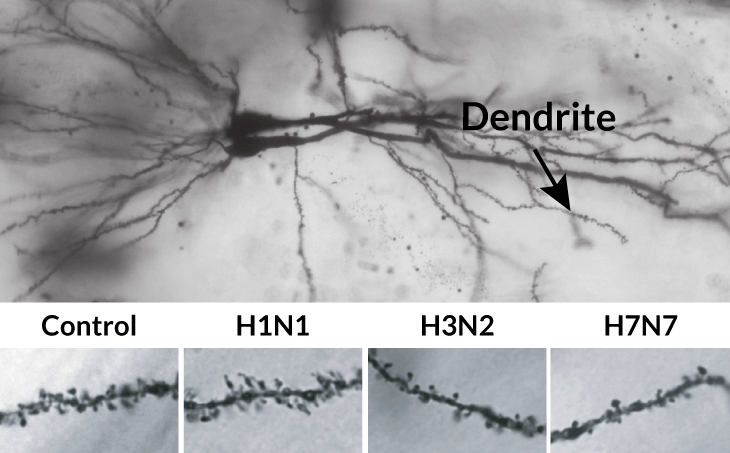
- Some flu strains can make mice forgetful. A team of German researchers have found that mice infected with certain strains of the flu experience memory loss after recovery. Three groups of mice were given a different strain of the flu virus with a fourth group given no virus to determine whether the brain was affected following infection. Upon recovery, the mice infected with H3N2 (2017-2018 flu) and H7N7 (a dangerous but rare strain) were not able to remember the location of a hidden platform in a test pool while the control group and those infected with the H1N1/ 2009 swine flu strain completed the task normally. They also found that the number of “message receiving” dendritic spines of nerves found in the brain were decreased in the mice that had the post infection memory loss. Memory function, however, eventually returned to normal. A researcher on the study, Martin Korte indicates that the results suggest that cognitive effects, in addition to lung function, should be monitored in people post-infection. Published in the Journal of Neuroscience.
- Scorpion venom compound may treat rheumatoid arthritis. Christine Beeton and her colleagues at Baylor College of Medicine found that iberiotoxin, one compound in scorpion venom, can reduce the severity of the disease in rats. Rheumatoid arthritis is an autoimmune disease that affects the joints. Cells called fibroblast-like synoviocytes (FLS) grow and move from joint to joint causing damage and attracting immune cells that cause inflammation and pain. Current treatments target the immune cells but none are specific for FLS. Beeton’s team found that iberiotoxin stopped an essential function in the FLS which reduced the severity of the rheumatoid arthritis in rats without side effects. Dr. Mark Tanner, a graduate student in the Beeton lab said, “It was very exciting to see that iberiotoxin is very specific for the potassium channel in FLS and that it did not seem to affect the channels in other types of cells, which might explain the lack of tremors and incontinence.” Published in the Journal of Pharmacology and Experimental Therapeutics.
- Human neural stem cells used to treat spinal cord injuries in primates. A study conducted at the California National Primate Research Center grafted human neural progenitor cells into primates that had been given spinal injuries. The neurons grew into up to 150,000 threadlike axons which bridged the injury and allowed the primates to better control their finger movements. This research builds on earlier studies in rodents and offers hope similar techniques could be used to treat human spinal injuries in the future. Published in Nature Medicine.

- Repeated anesthesia in infancy increases anxiety-linked behavior in nonhuman primates. Researchers at Yerkes National Primate Research Center, Emory University and Icahn School of Medicine at Mount Sinai found that monkeys that were repeatedly exposed to anesthesia during infancy showed anxiety-linked behaviors later in life when exposed to social stress. The reaction of monkeys is consistent to what is seen in human children meaning there is now an opportunity to understand the mechanisms of anesthesia-induced cognitive changes. First author, Jessica Raper, PhD, says. “If our current studies continue to add to the mounting evidence for neurocognitive effects after early anesthesia exposure, then our next steps will include studies to determine how to best protect the developing brain when anesthesia is required.” Published in the British Journal of Anaesthesia.
- Clinical trials for a stroke treatment developed in animals. Previous research in mice and pigs has demonstrated efficacy of a new stem cell treatment for stroke — with a 35% reduction in the size of the injury and a 50% reduction in brain tissue loss. Clinical trials are now planned in 2019, given these promising results. The treatment called AB126 uses extracellular vesicles (EV), fluid-filled structures known as exosomes — which are able to cross barriers that cells cannot. Published in Translational Stroke Research.
