Biological similarity of humans and other animals
Although humans and animals (technically “non-human animals”) may look different, at a physiological and anatomical level they are remarkably similar. Animals, from mice to monkeys, have the same organs (heart, lungs, brain etc.) and organ systems (respiratory, cardiovascular, nervous systems etc.) which perform the same functions in pretty much the same way. The similarity means that nearly 90% of the veterinary medicines that are used to treat animals are the same as, or very similar to, those developed to treat human patients. There are minor differences, but these are far outweighed by the similarities. The differences can give important clues about diseases and how they might be treated – for instance, if we knew why the mouse with muscular dystrophy suffers less muscle wasting than human patients, this might lead to a treatment for this debilitating and fatal disorder.
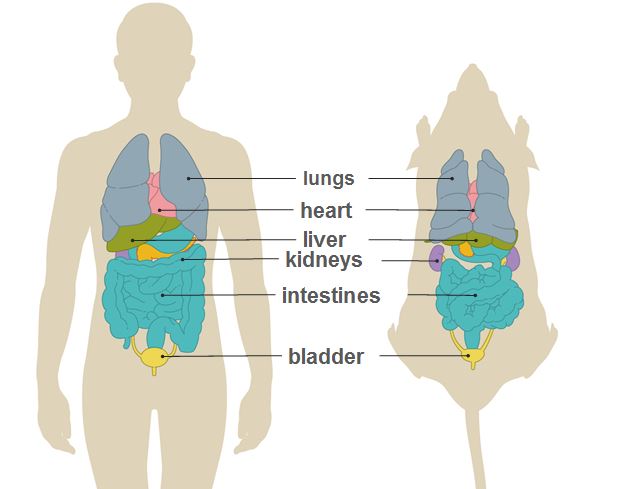
We share approximately 99% of our DNA with mice (1), and moreover, we can use “knockout” mice to work out what effect individual human genes have in our body. We do this by “turning off” one of the genes in a mouse, common to a human, and seeing what effect this has on the mouse. By recreating human genetic diseases in this way we can begin to look for treatments.
Nobel Prizes and animal research
For just over a century the Nobel prize has been awarded each year in recognition of the world’s greatest medical advances. Of the 108 Nobel Prizes awarded for Physiology or Medicine, 96 were directly dependent on animal research. Animal research underpinned the very first Nobel Prize to be awarded for Physiology or Medicine to Emil von Behring in 1901 for developing serum therapy against diphtheria, as it did the most recent awarded in 2016.
Animal model explained
The role of the animal model is neatly explained in “The Animal Research War”, by Michael Conn and James Parker (2):
If you are going to study a human disease you can’t, for ethical reasons, perform the initial work in humans; you have to develop a model. Some models may be in vitro – literally, in glass tubes – but as you learn more and more, you must eventually test ideas in vivo– in living animals. That means you have to have a way of producing the disease that allows you to study it.
Let’s consider AIDS, one of Podell’s interests. You could take its causative agent, the Human Immunodeficiency Virus (HIV), grow it in a test tube, and kill it by pouring bleach on it. Do you now have a way to kill HIV? Yes, you do. Do you have a treatment that can be used in humans? Absolutely not: bleach is toxic. Killing HIV in a test tube and killing it in a living animal are two very different accomplishments.
To complicate things further, viruses grow differently in test tubes than in humans. Humans have an immune system: test tubes do not. A virus growing in a test tube is not a good model for the human disease, but drugs that don’t kill the test tube virus probably won’t work in humans either – and these might be eliminated from further consideration.
Animal models allow closer approximation to a human response. They are not perfect, of course; animals host different diseases and different responses. While the fundamentals of life are the same – there is a 67 percent similarity between the DNA of humans and earthworms – there are differences in species and even in individual animals. Some animals are good human-like models for one thing and some for another; some have a cardiovascular system that is similar to humans while others have similar skin.
Current examples of animal research in medicine
Find hundreds of examples of how animal studies have contributed to medical breakthroughs, please see our Research Index, which lists all our posts categorised by either the species involved, or the disease addressed.
—
(1) – “The measure of man” – http://www.sanger.ac.uk/Info/Press/2002/021205.shtml
(2) – Conn, P.M. & Parker, J.V., 2008, The Animal Research War, Palgrave Macmillan

