March 21st 2022
Jeremy D. Bailoo
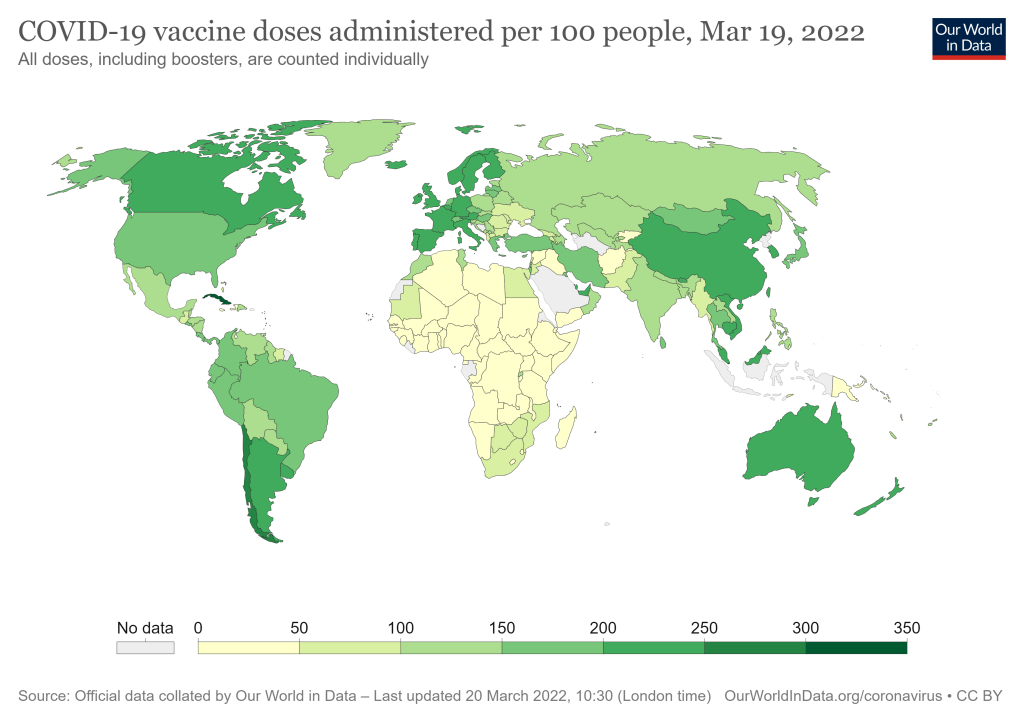
While some countries appear to be emerging from the pandemic, many developing countries continue to struggle to vaccinate their citizens because they have limited access to the vaccine. Now, thanks to animal research, an inexpensive, easy-to-store, and effective alternative to RNA vaccines—a protein subunit vaccine—may be on the horizon.
The researchers report that the protein subunit vaccine, which comprises fragments of the SARS-CoV-2 spike protein placed on a virus-like particle, elicited a strong immune response and protected animals against viral challenge.
“In places in the world where cost remains a challenge, subunit vaccines can address that. They could also address some of the hesitancy around vaccines based on newer technologies,” Love, author of the article, says. Other widespread subunit vaccines include those for hepatitis B and acellular pertussis.
Another advantage of protein subunit vaccines is that they can often be stored under refrigeration and do not require the ultracold storage temperatures that RNA vaccines do.
For the subunit vaccine, the researchers decided to use a small piece of the SARS-CoV-2 spike protein, the receptor-binding domain (RBD). Early in the pandemic, studies in animals suggested that this protein fragment alone would not produce a strong immune response, and so the team decided to display many copies of the protein on a virus-like particle (a scaffold). They placed the SARS-CoV-2 RBD fragment on a scaffold created by the body when exposed to Hepatitis B (an antigen) and showed that when coated with SARS-CoV-2 RBD fragment, this particle generated a much stronger response than the RBD protein on its own.
Once the researchers had their vaccine candidate ready, they tested it in a small trial in nonhuman primates. For those studies, they combined the vaccine with a substance that enhances the body’s immune response (adjuvant) and which is commonly used in other vaccines: either aluminum hydroxide or a combination of alum and another adjuvant called CpG.

In those studies, the researchers showed that the vaccine generated antibody levels similar to those produced by some of the approved Covid-19 vaccines, including the Johnson and Johnson vaccine. They also found that when the animals were exposed to SARS-CoV-2, viral loads in vaccinated animals were much lower than those seen in unvaccinated animals.
For the vaccine mentioned above, the researchers used an RBD fragment that was based on the sequence of the original SARS-CoV-2 strain that emerged in late 2019. That vaccine has been tested in a Phase 1 clinical trial in Australia. A Phase 1 clinical trial is a test in less than 100 human adult volunteers. Since then, the researchers have incorporated two mutations (similar to ones identified in the natural Delta and Lambda variants) that the team previously found to improve production and immunogenicity compared to the ancestral sequence, for the planned Phase 1 and Phase 2 clinical trials. A Phase 2 clinical trial is similar to Phase 1 trials, but with a few hundred human adult volunteers.
The vaccine was designed so that it can be produced by yeast, using fermentation facilities that already exist around the world. The Serum Institute of India, the world’s largest manufacturer of vaccines, is now producing large quantities of the vaccine and plans to run a clinical trial in Africa.
If the clinical trials show that the vaccine provides a safe and effective alternative to existing RNA vaccines, the researchers hope that it could not only prove useful for vaccinating people in countries that currently have limited access to vaccines. They also hope that it would lay the foundation for creating boosters that offer protection against a wider variety of SARS-CoV-2 strains or other coronaviruses. That is important because what the last 3 years have taught us is that being prepared saves lives!
**Content taken from press release and edited for style
