Hot on the heels of last weeks report of the successful use of gene therapy to treat the eye disease Leber’s congenital amaurosis comes a report that scientists lead by Nathalie Cartier and Patrick Aubourg of the French National Institute for Health and Medical Research have combined gene therapy and stem cell medicine to successfully treat two boys with the disease cerebral X-linked adrenoleukodystrophy (X-ALD).
What is X-ALD?
X-ALD is caused by mutations in the ABCD1 gene that plays a key role in the transport of fatty acids within cells, and lack of ABCD1 causes long-chain fatty acids to build up within cells known as microglia and oligodendrocytes in the brain. Affected microglial cells and oligodendrocytes eventually cease to maintain the insulating myelin sheath that is required for effective transmission of electrical impolses along nerve cells, leading to brain damage and ultimately death at an early age. The disease was made famous by the film “Lorenzo’s oil” which describes a dietary supplement that may delay the progression of the disease, though the only treatment that is currently considered truly effective is allogeneic hematopoietic cell transplantation where healthy bome marrow stem cells from a donor are transplanted into the X-ALD patient.
Allogeneic hematopoietic cell transplantation works because the microglial gells and oligodendrocytes develop from cells that migrate to the brain from the bone marrow, so that healthy cells from the donor eventually replace some of the patient’s ABCD1 deficient cells and help maintain the myeline sheath. Unfortunately it is often difficult to identify a suitable donor, and even if one is found the procedure is risky due to problems such as graft-versus-host disease where immune cells in the donated bone marrow mount an immune response against the patient’s tissues.
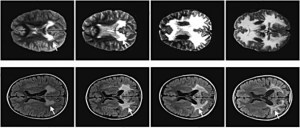
Mice and the development of gene therapy for X-ALD
Dr. Cartier and colleagues examined the possibility of using gene therapy to modify the patient’s own hematopoietic stem cells so that they express a functioning ABCD1 gene and then injecting these cells into the patient to replace their faulty bone marrow hematopoietic cells, thereby avoiding the problem of donor and host incompatability. Rather than attempt to genetically modify and transplant all types of human bone marrow stem cells they concentrated on a subset of cells called the CD34+ cells that give rise to many cells of the immune system. These have the great advantage that they can be isolated from the blood, avoiding the need for surgery to harvest bone marrow.
To assess whether genetically modified CD34+ cells could develop into cells of the immune system when injected into the bone marrow they selected the NOD/SCID mouse that lacks a functioning immune system and is often used to assess human stem cell transplantation techniques and to study aspects of the human immune system. Initial results with retroviral vectors were disappointing but using the NOD/SCID mouse model they developed a lentiviral vector based on HIV-1 that enables the functioning ABCD1 gene to safely incorporate into the genome of a significant proportion of the cells and drive ABCD1 expression in immune system cells derived from them (1). What is more they found that as well as the expected range of immune cells the genetically modified CD34+ cells migrated to the brain and differentiated into microglial cells (2). Of course if the therapy is to prevent disease progression the vector needs not only to drive expression of ABCD1 but to do so reliably for many years,. To assess whether the lentiviral vector could do this they transplanted Sca-1+ cells, the mouse equivalent of human CD34+ cells, containing the ABCD1 expressing lentiviral vector into mice that lacked a functional ABCD1 gene, and found that even 12 months after transplantation almost a quarter of microglial cells in the mouse brain expressed ABCD1 (3).
From mice to human trials
These promising results in mice were enough to persuade Dr. Cartier and her colleagues that this therapy should proceed to a pilot study in human patients who are in the early stages of this desease. While it will take several years of observation and clinical trails involving larger numbers of patients before we can be sure that this therapy is a success, this exciting news is yet another sign that gene therapy is finally coming of age.
Paul Browne
1) Benhamida S. et al “Transduced CD34+ cells from adrenoleukodystrophy patients with HIV-derived vector mediate long-term engraftment of NOD/SCID mice.” Mol Ther. Volume 7(3), pages 317-324 (2003) PubMed: 12668127
2) Asheuer M. et al. “Human CD34+ cells differentiate into microglia and express recombinant therapeutic protein” Proc Natl Acad Sci U S A. Volume 101(10), pages 3557–3562 (2004) PubMed Central: PMC373501
3) Cartier N. et al. “Hematopoietic Stem Cell Gene Therapy with a Lentiviral Vector in X-Linked Adrenoleukodystrophy” Science Volume 326(5954), pages 818 – 823 DOI: 10.1126/science.1171242
