Earlier today we posted a commentary on PeTA’s misleading propaganda by Professor Anthony Garro of UMass Dartmouth. At the time I mentioned that it was a pity that Prof. Garro was not able to write more about the role of animal research in 21st century medicine, but a recent story in Nature News provides an excellent example, showing how research on mice and monkeys was crucial to the development of a new drug for lupus.
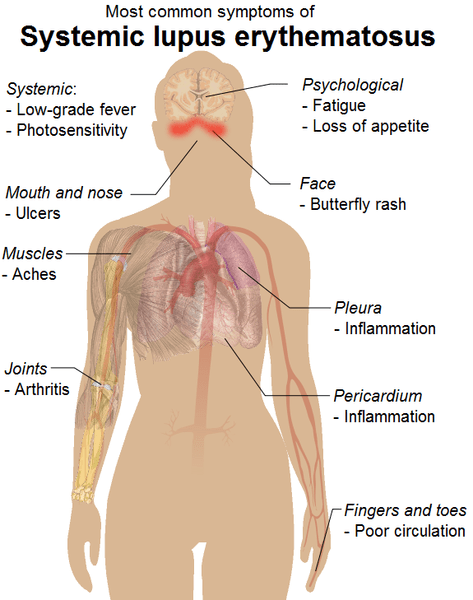
The autoimmune disease lupus, or to give it its full name Systemic Lupus Erythematosus (SLE), affects over 100,000 people in the United States, causing damage to a variety of tissues in the body and a wide range of symptoms ranging from fever, headache and joint pains to anemia and renal failure. While there is no cure for lupus it can be treated successfully, though current treatments do not work well for all patients.
A couple of weeks ago there was a significant advance in the treatment of Lupus, with the approval by the FDA of first new drug specifically for lupus in 50 years. As the Nature news article reports, Benlysta (belimumab) works by binding to and inhibiting a protein called the ‘B-lymphocyte stimulator’ (BLyS),. This causes the immune system’s antibody-producing B lymphocytes to self-destruct, thereby reducing the body’s ability to attack its own tissues. Benlysta is one of the first drugs to come out of the human genomics revolution that has transformed medical research over the past two decades, and the Nature News article quotes David Hilbert, one of the scientists involved in the research on gene expression in B lymphocytes that led to the development of Benlysta as saying.
You’d sit there and watch new genes coming off the line every day and you didn’t know what they were and what they did,”
So how did they find out what BLyS does and whether blocking it would help in lupus? This is where animal research came in, specifically research involving genetically modified mice which allowed scientists to determine the role that BLyS plays in B-cell proliferation and in autoimmune diseases. An article published in the journal Arthritis and Rheumatism in 2003 describes the early work on Benlysta (then called LymphoStat-B)
In vivo, recombinant human BLyS causes splenic hyperplasia in mice, primarily due to increases in the number of mature B cells. BLyS administration to mice also causes increases in the total serum Ig concentration and enhanced humoral responses to both T cell–independent and T cell–dependent antigens (1, 2, 8).
BLyS has been shown to bind with high affinity to 3 receptors, all of which are members of the TNF receptor family (6, 9, 10). Two of the receptors, BCMA and TACI, also bind APRIL, another TNF family member that is the most homologous to BLyS (11–13). The precise function of these two receptors is not well understood, but studies in knockout mice suggest that BCMA is functionally redundant, since BCMA-deficient mice have a normal B cell phenotype (14). TACI has been shown to have an inhibitory role in B cell development, since TACI knockout animals exhibit increased peripheral B cells, reduced responses to T cell–independent antigens (15, 16), and lymphoproliferative disorders and autoimmune disease (17). In contrast, BLyS-deficient mice show a phenotype of severe loss of mature B cells in the spleen, peripheral blood, and lymph nodes (18, 19). A third receptor, BLyS receptor 3 (BR-3; BAFF-R), is specific for BLyS (9, 10). The A/WySnJ mouse strain, which harbors a naturally occurring truncation of BR-3, exhibits a phenotype similar to that of BLyS-deficient mice (9, 10, 20), suggesting that BR-3 is the primary mediator of the effects of BLyS on B cell survival and maturation.
Several lines of evidence suggest that elevated levels of BLyS may be involved in the pathogenesis of B cell–mediated autoimmune diseases. First, constitutive overexpression of BLyS in transgenic animals results in manifestations of autoimmune-like symptoms, including anti-DNA antibodies, rheumatoid factor, circulating immune complexes, and deposition of immune complexes in the kidney leading to glomerulonephritis. These symptoms resemble those of systemic lupus erythematosus (SLE) and some aspects of rheumatoid arthritis (RA) (21, 22). Second, elevated levels of BLyS have been found in other murine models of SLE, including MRL-lpr/lpr and (NZB × NZW)F1 strains (6). Finally, elevated levels of BLyS have been observed in the serum of patients with SLE and RA (23, 24) as well as Sjögren’s syndrome (25, 26). Significant correlations between BLyS levels and autoantibody production were shown in these studies.
The association of BLyS overproduction with manifestations of several autoimmune diseases suggests that modulation of BLyS levels could be a novel therapeutic approach to the treatment of such diseases. Indeed, studies with soluble BLyS receptors as antagonists have shown efficacy in reducing disease manifestations in murine models of both SLE and RA (6, 27, 28). With the aim of developing a therapeutic agent for autoimmune disease, LymphoStat-B (Human Genome Sciences) antibody, a human, neutralizing monoclonal antibody against human BLyS, was generated. We describe herein the generation of human antibodies against BLyS using phage display, as well as the in vitro and in vivo characterization of LymphoStat-B.”
This basic research underpinned the subsequent development of an antibody-based therapy to treat lupus, but it wasn’t the only crucial contribution animal research made to the development of Benlysta. During the final pre-clinical stages of its development the effectiveness of Benlysta was evaluated in a GM mouse model of lupus where the mouse BlyS gene was replaced with its human counterpart, and also for its broader effects on the immune system of in cynomolgus monkeys, since in vitro studies had determined that the effect of Benlysta on the cynomolgus monkey BLyS gene is very similar to humans. These studies supported the effectiveness and safety of Benlysta and enabled clinical trials to begin.
The development of Benlysta is a great example of how research in animals goes hand-in-hand with human genomic studies, and clinical research in allowing scientists to develop important new treatments for diseases that affect many thousands of people. As the Nature News article points out Benlysta does not work for all lupus patients, something that would be expected with such a variable disease, but this is only the start, several other promising lupus drugs are in the pipeline, and with luck they will soon add to the list of efffective treatments available for this disease.
This is what Professor Garro and many other scientists are now standing up for!
Paul Browne
