April 19th, 2021
Professor Christopher Petkov
Although we have been focusing on updates on Covid-19 vaccines and their reliance on research with nonhuman animals including primates (as an example post see here), two other developments focusing on treatments for AIDS and Zika fever have caught our eye.
These fall under the topic #MPAR, Made Possible by Animal Research.

Permanently stopping the HIV virus
The Acquired Immunodeficiency Syndrome (AIDS) is caused by the Human Immunodeficiency Virus (HIV) and its variants. If an individual is infected with this blood-borne virus, the virus leads to severe immune system deficiency which could be fatal. AIDS makes the person vulnerable to diseases that are otherwise well controlled by the immune system.
Current treatments for AIDS include antiviral medication that needs to be taken throughout a person’s life to keep the virus at check. Taking antivirals for such a long time can have side effects. However, the antivirals can be very effective in keeping the virus at bay, both reducing the likelihood of the disease occurring and the virus being passed to others.
Other treatments involve vaccines that either help to protect the individual from getting HIV or are therapeutic in people that have HIV to reduce their reliance on antiviral medication. The problem is that the HIV viruses, like all viruses, regularly change or mutate. These changes by the virus can sometimes give it the ability to escape an otherwise effective vaccine against other variants. Thus scientists need to stay vigilant and to regularly obtain scientific information on how vaccines could be updated to help the body to fight off viruses.
There is also a need to better understand how to boost the virus fighting responses by the body, thereby making vaccines more effective. For instance, there is still the hope that a highly effective HIV vaccine that helps immune cells, like T-cells to destroy body cells infected with the virus, could potentially get rid of the virus entirely from an infected person.
This ongoing process of vaccine development and refinement relies on #animalresearch and as such can be labelled #MPAR.
Animal research can also provide information on the safety and likely side effects of the potential vaccines, as well as information that cannot be obtained in humans about the impact of the disease on body cells or how the vaccines work.
The animal research does, however, need to be closely linked to the human variants of the disease (HIV), which can be done via testing that compares effects in both the nonhuman animals and humans. For instance, monkeys are affected by the monkey variants of the virus known as the Simian Immunodeficiency Viruses (SIV). However, virus variants are not identical, requiring the additional step of making the direct comparison to the human HIV variants. Rather than assuming that because the vaccine is effective in monkeys that it will also work in humans, this assumption needs to be scientifically tested. There are also multiple types of human variants of HIV, which may require different vaccines for each human variant.
This ongoing scientific effort underscores the need for effective animal models and research may continue even years after the first set of vaccines have been developed. It also highlights the need for scientists to explore different vaccine options, including better understanding the ways in which vaccines work and how safe they are, whereby a research with relatively few animals can make a large positive impact on human medicine and health.
Breakthrough in vaccination efforts for HIV
Researchers at Oregon Health Sciences University recently published several scientific papers reporting on an improved potential treatment for SIV and establishing the link to human HIV. Their approach is based on a highly effective cytomegalovirus (a modified beneficial version of a Herpes virus). By understanding how the vaccine works and how it can be modified to be more effective against SIV in monkeys, the scientists obtained evidence suggesting it is likely to be highly effective with HIV, also establishing the scientific bridge to humans along the way by modifying the vaccine in ways needed to be effective against HIV.
This exciting news is a direct consequence of research with nonhuman primates for a disease that since its inception has claimed over 34 million lives.
This promising improved vaccine may now enter clinical trials for it to be assessed for effectiveness. Even if the vaccine being tested is found not to work as well as had been hoped in the clinical trials, the animal research bases established will help expedite future modifications and improvements to the vaccine.
Thus, #animalresearch will continue to be an important part of the scientific bedrock that both supports the current potential treatment and leads to future ones, even if not every scientific study with research animals leads directly to a clinical trial in humans.
A Zika virus vaccine moves to preclinical testing
The Zika virus is spread by mosquitoes and causes mild to no symptoms, but it can result in severe birth defects in the baby of a pregnant woman infected with it. That is not to say that there is little impact on the infected person, because some people infected with the Zika virus can suffer from disorders like Guillain-Barre Syndrome, whereby the immune system attacks the peripheral nervous system affecting the person’s ability to move and feel. Currently there are a number of potential Zika virus vaccines in clinical trials.
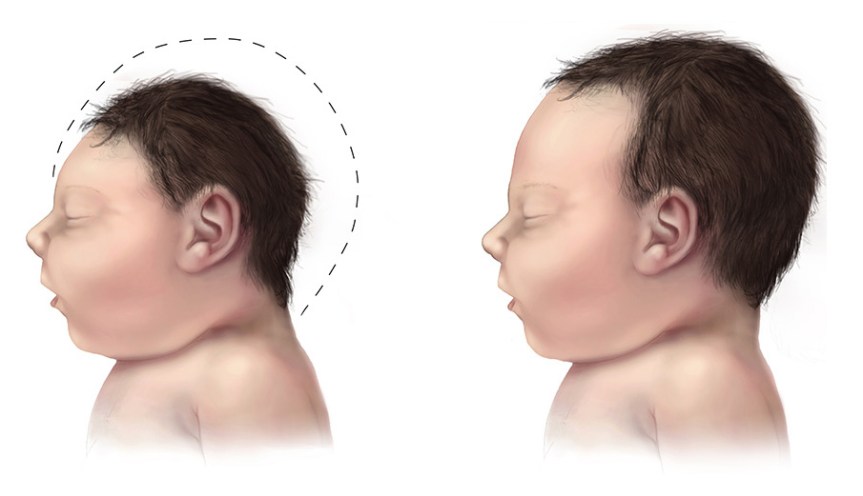
The University of Connecticut recently reported on a Zika vaccine that is in preclinical studies. The scientists used the genetic sequence of the virus to create virus-like particles. Introducing these particles into the body as a vaccine may boost the immune response against the virus, and thus protect the individual from getting infected with Zika.
Using virus-like particles makes the vaccine safer in that the particles themselves are biologically engineered not to cause infection. This strategy is similar to some of the Covid-19 vaccines that were developed to introduce a spiny protein of the Covid-19 virus to spur the immune system to fight off the viral infection, but which by itself will not harm the body.
The University of Connecticut scientists tested the efficacy of the Zika vaccine in mice. The results in their preclinical studies with the mice were promising and now have the potential to lead to clinical trials in humans to assess their effectiveness in people.
At a time when because of the Covid-19 pandemic we are finally starting to see the number of lives lost to the disease substantially decrease because of preventative and vaccination efforts, these new developments give us confidence in scientists working for global benefit.
The scientific benefits involving animal research will be a relief not just for Covid-19 containment efforts but also for the many other diseases that affect millions of people, such as those caused by the HIV and Zika viruses.
