March 9th 2021
Sangy Panicker, Allyson J. Bennett, Amanda M. Dettmer, Justin A. Varholick, Jeremy D. Bailoo
The world has faced an unprecedented crisis in the COVID-19 pandemic, with 113.5 million cases and over 2.5 million deaths globally since the start of the pandemic. Scientists across the globe, in diverse and sometimes disparate fields, have come together in a once in a lifetime manner to combat this crisis. This global scientific enterprise resulted in various vaccines receiving Emergency Use Authorization. In the US, the rollout of three vaccines, Pfizer-BioNTech, Moderna and Janssen holds promise to an end to what has been a decidedly terrible year. Now, more than ever we are reminded of the vital role that animal research plays both in basic research, such as in understanding immune system regulation, and applied research, where that knowledge is used in the development of cures and other therapeutic strategies.
While scientific experts are working diligently to combat the COVID-19 virus anti-animal research groups were exploiting this devastating pandemic to push its agenda and fill its coffers—unsurprising as, for example, PETA in 2019 reported ~5 million dollar operating loss from its 55 million dollar budget. With respect to animal research and animal researchers, the issues commonly raised are more often than not at best without merit, or at worst, contrived and sensationalized to elicit maximum emotive value. At Speaking of Research, we have worked diligently to highlight these issues and to provide the public with the necessary context when needed. Below we highlight what those opposed to animal research are doing while the scientific community is trying to save lives.
The decision to humanely euthanize research animals and prioritize human life
The COVID-19 pandemic resulted in a global lockdown of in-person activities and subsequently social distancing and other mandates. In the United States, this lockdown coincided with the week long Spring Break holiday for many universities. Here, universities and researchers were faced with an unprecedented challenge—to protect the safety of researchers, lab animal care staff, and other frontline workers—and decide within an extremely short time (< 2 weeks and in many cases as little as 48 hours) which animals should be kept and which animals should be humanely euthanized.
One might ask, why were these decisions necessary? Given the many unknowns of the COVID-19 virus at the start of the pandemic, researchers in particular and universities in general were anticipating that care-staff could become infected, that the risk to human life from in-person research and other activities would be immense, and that the possibility of zoonotic transmission was very real. Importantly to safeguard our frontline workers such as nurses and doctors, the decision was made to donate all of the personal protective equipment (PPE) that could be spared to healthcare and other essential workers. Here, it is important to remember that at the start of the pandemic (~March 2020), many countries, including the United States, experienced a shortage of PPE. What many people do not realize is that this shortage continues, even today, and our priority rightfully continues to be the distribution of PPE to our frontline health care and other essential workers.
As a consequence of the many unknowns a year ago—including our decision as a society to safeguard and prioritize human life first as well as the anticipation that this pandemic could rage on for at least a year—some researchers and universities had to make the difficult decision to humanely euthanize animals. Mice are the most prevalently used animal for research and therefore were the great majority of animals that were euthanized. These decisions were not taken lightly, and researchers, for example, prioritized mouse lines that could not otherwise be easily replaced.
These actions were taken to ensure both the safety of staff and the welfare of the remaining animals in their care. Given the possibility of veterinarians, technicians, and other workers getting sick or being forced to stay at home, lab animal facilities needed to make sure that they had the resources to feed, clean, and provide medical care to thousands of animals.
#AnimalResearch shaped our timely response to the COVID-19 pandemic
Like so much of #AnimalResearch, the #timescales from bench to bedside are often long, making it difficult to grasp the immediate human benefit of such research. Take for example the fact that in the US, we were able to produce three vaccines in ~1 year that have received Emergency Authorization Use for COVID-19. How was such a feat managed? As we wrote about at the start of the pandemic, such rapid progress was possible because of #AnimalResearch over the past decade into coronaviruses, which included Severe Acute Respiratory Syndrome (SARS) and the Middle East Respiratory Syndrome (MERS), along with decades of prior research into mRNA vaccines.
Generally, the safety and efficacy of all vaccines (just like all other medications) are tested in animals before making their way to clinical (human) trials. Because of the urgency of the COVID-19 threat, however, safety and efficacy testing for some of the 160 candidate vaccines and treatments developed (e.g., Moderna’s mRNA-1273 vaccine) were fast-tracked and Phase 1 clinical trials began—where typically the lowest number of human subjects are enrolled. That is not to say that safety and efficacy was not evaluated pre-clinically in animal models for those candidates, however. Instead, safety and efficacy was being evaluated in animals in tandem with human trials, rather than prior to human trials.

Other animal species, such as monkeys, cats, dogs, ferrets, chickens, and even horses are being used in our fight against COVID-19 to address pertinent questions such as:
- Do animals develop immunity after vaccination and infection?
- If they do develop immunity, for how long?
- Are there species differences?
- What does that immune response look like?
- Do any vaccine candidates elicit unwanted effects?
What those opposed to animal research were doing
While scientists were hard at work and prioritizing human life amidst the pandemic, anti-animal research groups, such as PETA, used the inevitable decision to euthanize some research animals combined with the circumventing of the accepted research practice of doing preclinical studies before testing potential cures and vaccines in humans, to tout the false claim that it proves animal research is nonessential. Ironically, its mission to misinform the public was supported by taxpayer dollars by applying for and receiving federal funds for pandemic assistance to pay employees (PPP under the CARES Act).
At the same time, irresponsible protests were organized as part of their anti-animal research agenda. Protestors, some of whom were seen devoid of personal protective equipment like face masks, were driving through neighborhoods, screaming at residents, honking their car horns and even getting out of their vehicles to confront police and local residents, placing everyone’s health and safety at risk.
Those opposed to animal research also inundated government agencies with requests to “recover government funds” because many labs had to prioritize human life, which consequentially led to the humane euthanasia of some animals (as detailed above). PETA sent letters to no fewer than 10 government agencies. The letters were all similar in theme—one letter to NIH Office of Management Assessment read:
“According to new documents received so far by PETA through Freedom of Information Act requests, we confirmed that the following universities have euthanized animals deemed unnecessary, non-essential, extraneous, or surplus or described using any other similar language in response to university ramp-down directives due to the COVID-19 pandemic.”
Nowhere in these letters is there adequate context, as we have provided above, with respect to the decision making process engaged in by individuals and institutions involved with animal research. Rather the complaint was based on the usual singular ideological focus that animals should not be used for any purpose by humans. With animal research paving the way for the three vaccines that have received Emergency Use Authorization in the US, the hypocrisy of those opposed to animal research willingly taking the vaccine continues to astound us all.

The need to build capacity for the next pandemic
Part of the reason why the traditional approach of preclinical studies preceding clinical research was circumvented in the pandemic related to the fact that the traditional animal model used in initial tests, the laboratory mouse, does not naturally get sick from the coronavirus. A special mouse was therefore needed—one that contains human genes—a “humanized” mouse. Such a mouse existed, and was created during the SARS epidemic, ~16 years ago. This mouse contained the human ACE2 gene and was developed by researchers at the University of Iowa. Sperm from these mice were cryopreserved, and these sperm were sent to the Jackson Laboratories for recovery and mass production. The process from “unfreezing” to breeding, and waiting for the animals to grow before they could be used in experiments took approximately 12 weeks (3 months). After that, experiments began, which took months to complete.
With respect to COVID-19, the question of suitability of the animal species for model development, particularly in a time of crisis bears scrutiny. Here, there was a need for an animal species that naturally developed COVID-19, so that research could begin immediately—non-human primates were the most relevant animal species to fill this need. Probabilistically, it is also most likely that non-human primates will be the most relevant species for addressing emerging health threats. Moreover, prior to therapeutics being used in humans, safety and efficacy tests are conducted in various animals—of which non-human primates are prioritized given their similarity to humans.
It is here, however, that scientists in the United States say they are facing a bottleneck. There just aren’t enough monkeys to meet the biomedical demand for this pandemic, to say nothing of the countless other diseases that still remain untreated and uncured. According to the Atlantic the reasons for the shortfall are threefold:
“First, COVID-19 has created extraordinary demand for monkeys. Second, this coincided with a massive drop in supply from China, which provided 60 percent of the nearly 35,000 monkeys imported to the U.S. last year and which shut off exports after COVID-19 hit. And third, these pandemic-related events are exacerbating preexisting monkey shortfalls.”
In other words, countries which support research on drug discovery for existing and emergent diseases, such as COVID-19 and its variants, need to build up a strategic reserve of non-human primate animals to effectively prepare for the next pandemic, which some epidemiologists have argued is inevitable.
In addition to the shortfall in animals, infrastructure investments need to be made so that the research capacity can be maximised. One of the glaring shortages in the ongoing COVID-19 pandemic was the very limited number of Bio-Security Level 3 (BSL-3) laboratories—BSL-3 laboratories are appropriate for work involving microbes which can cause serious and potentially lethal disease via the inhalation route. There are approximately only 1,376 BSL-3 laboratories in the US.
The US also needs to match R&D investment pace if it aims to be a global leader in science. For example, China has recognized the need for fundamental research (basic research) and is increasing its investment by 10% in this area. Basic/Fundamental research is the reason we had a leg-up on the COVID-19 virus—over a decade of research into similar coronaviruses which includes Severe Acute Respiratory Syndrome (SARS), Middle East Respiratory Syndrome (MERS) and many decades of research into immune system regulation and the like.
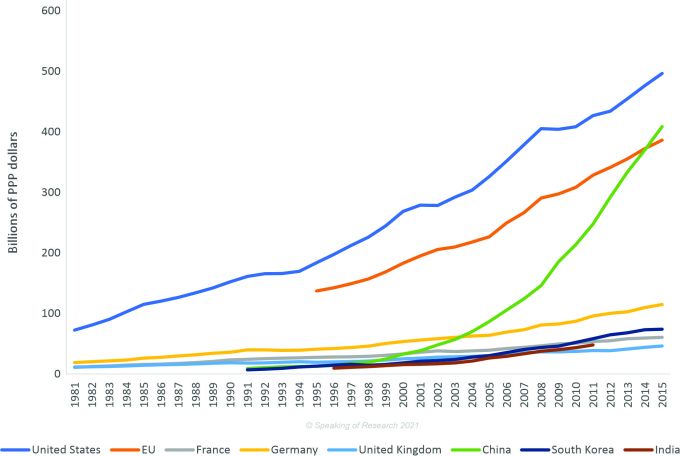
**EU = European Union; PPP = purchasing power parity.
The numbers of animals used for research during the pandemic will likely have decreased
We anticipate that for all of the reasons listed above the total numbers of animals used for research will have decreased in 2020 and potentially in 2021. That decrease is unlikely to be reflected when animal use statistical reports are released. Why? Because the most prevalently used animal for research, the mouse, is not covered under the Animal Welfare Act (AWA), and thus not included in statistical counting. Despite their lack of inclusion in the AWA, the welfare for mice used in research is assured via PHS Policy and OLAW—a fact that we have addressed many times over. Based on animal use statistics from other countries which do include mice in their statistical counts, we estimate that 93% of all animals used for research are mice. Given the prioritization of human life during the pandemic, the fact that research with animals was paused, and that mice were most likely to have been humanely euthanized, then the number of animals used for research will have decreased in 2020. In contrast, however, given that dogs, cats, and non-human primates are covered by the AWA, and thus counted in annual use statistics, and that these species were used for the development of therapeutics for COVID-19, we predict that animal use will appear to have increased in 2020, despite actually decreasing.
As we’ve written about before, the collection of statistical data on animal use are undoubtedly useful for some purposes but they also have major limitations with respect to informing meaningful and serious consideration of the ethical use of animals in research. Simply reporting the numbers ignores the global context and relevant information about fluctuations in animals used in research over time. As a result, however, such reporting can often fall short of the overall goal. A perfect example would be the impact of the COVID-19 pandemic on biomedical research. At SR we believe that a key goal of transparency is to provide not only accurate information, but also the meaningful context that can inform serious consideration and decisions about global science, medical advances, and public benefit. When animal use numbers are eventually released, we will aim to provide a nuanced description of this context and we hope that others interested in serious consideration of animal use numbers do the same.

