Brain metastasis that affect at least 20% of cancer patients are a serious problem for doctors seeking to treat cancer and kill thousands of patients every year, being particularly difficult to treat because many anti-cancer drugs cannot cross the blood-brain barrier and because surgery to remove the tumor can often be difficult and risky. Patients suffering from breast, lung and skin cancer run a relatively high risk that their cancer will spread to the brain, a worrying fact considering that these are amongst the most common of cancers . As a consequence of this scientists are very keen to understand how cancer spreads to the brain, with the ultimate aim of preventing that spread.
It has long been thought that brain metastasis is due to interactions between cells that are shed by the primary tumor and the nerve cells of the brain, but real evidence of this from living animals and humans for that theory has been hard to find, and in recent years observations made in animal models of cancer have suggested that blood vessels in the brain rather than nerve cells are the site of the early growth of tumor cells during brain metastasis. This week a paper in the open access journal PLoS One reports on work done by scientists at Oxford University that confirms that during brain metastasis tumor cells do indeed bind to blood vessels and form tumors before spreading into the surrounding nerve tissue, a result of huge importance to the future treatment and prevention of brain metastasis.
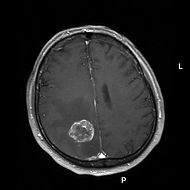
To demonstrate this Dr Shawn Carbonel and colleagues (1) injected breast and skin tumor cells into the bloodstream or fat tissue of mice and then after several days humanely killed the mice determined where in the brain the micrometastases, small colonies of tumor cells that later grow into tumors, were forming, and found that almost all were associated with the blood vessels. There was no sign of any new blood vessel growth, which indicated that the metastases were associating with the blood vessels, and that it wasn’t simply the case that they were promoting the growth of new blood vessels in the vicinity of the growing tumor. To confirm that this is also true in humans they examined tissue samples that been donated following neurosurgery or autopsy and found that almost all metastases were associated with blood vessels, a finding that supported the results of their experiments in mice.
Now they had to answer a new question; were the micrometastases associated with the blood vessels because they have a preference for interacting with the cells of the blood vessel, or simply because the first part of the brain they come to is that adjecent to the blood vessel? To answer this the Oxford scientists injected tumor cells that were labelled with green fluorescent protein directly into an area of the brain allowing equal access to both blood vessels and nerve cells, and using a cranial window in the skulls of the mice were able to observe where the GFP-labelled tumor cells ended up. They observed that the GLF-labelled cells associated almost exclusively with blood vessels, and that the tumors subsequently grow into the surrounding brain tissue.
The tumor cells bind to a blood vessel structure called the vascular basement membrane (VBM), but what the Oxford scientists really wanted to know was what caused the tumor cells to bind to the VBM. Once again using mice with cranial windows fitted they found that an enzyme named focal adhesion kinase was highly active where the tumor cells were interacting with the VBM. Focal adhesion kinase is part of a pathway through which a class of proteins known as the integrins control the interaction between many cells and either other cells or extracellular proteins such as the components of the vascular basement membrane, an observation which suggested that an integrin plays a key role in the binding of tumor cells to the VBM. They next found that a particular integren named Beta 1 integrin is present on all the tumor cell lines they were studying, and that antibodies blocking it could prevent the tumor cells from binding components of the VBM in vitro and to blood vessels in human brain tissue slices.
But would the anti-Beta 1 integrin blocking antibody prevent tumor metastasis in living animals? The answer was yes, the antibodies greatly reduced the growth tumors from human breast tumor cells that were injected directly into the brains of mice. To further emphasize the importance of Beta 1 integrin in brain metastasis they found that when mouse lymphoma cells that had been genetically engineered to lack Beta 1 integrin were injected into mouse brains they formed far smaller tumors than non-GM lymphoma cells.
This study changes the way we look at the process of brain metastasis, and more importantly in Beta 1 integrin it identifies a target for new drugs, perhaps monoclonal antibodies, that block the binding of tumor cells to blood vessels and prevent brain metastasis. With this in mind it is useful to note that studies in mice have found that while Beta 1 integrin is crucial during embryonic development prolonged anti-Beta 1 therapy in adult animals did not produce any overt evidence of toxicity (2), indicating that it should also be possible to inhibit it safely in human patients during anti-cancer chemotherapy.
It’s a very nice paper, my only gripe being that they didn’t examine if anti-Beta 1 integrin blocking antibody therapy could prevent tumor cells injected into the mouse bloodstream from producing micrometastases in the blood vessels of the brain rather than just looking at the growth of tumor cells injected directly into the brain, though I expect that those experiments are now being done and will soon be reported. There will certainly be a lot of interest in this paper in the cancer research world, and scientists will seek to reproduce these results (a vital part of the scientific process) and then expand on them with their own studies of the safety and efficacy of this approach before clinical trials in humans can begin.
Regards
Paul Browne
1) Carbonell W.S. et al. “The vascular basement membrane as “soil” in brain metastasis.” PLoS ONE Volume 4(6):e5857 (2009) DOI:10.1371/journal.pone.0005857
2) Park C.C. et al. “Beta1 integrin inhibitory antibody induces apoptosis of breast cancer cells, inhibits growth, and distinguishes malignant from normal phenotype in three dimensional cultures and in vivo.”Cancer Res. Volume 66(3), Pages 1526-1535 (2006) DOI:10.1158/0008-5472.CAN-05-3071

This isn’t the only interesting cancer research news this week, the BBC reports that scientists from the University of Heidelberg have made an important discovery about the role played by signalling proteins granulocyte- and granulocyte-macrophage colony-stimulating
factors (G-CSF ans GM-CSF) in the often severe pain associated with many cancers. Cancer pain has long been known to be different to other kinds of pain, and is difficult to treat
http://news.bbc.co.uk/1/hi/health/8089306.stm
G-CSF and GM-CSF are known to play a role in the development of blood cells, but Dr. Matthias Schweizerhof and colleagues were surprised to find high levels of these proteins in the pancreas of pancreatic cancer patients, and that nerves in this tissue had the receptors that bind them.
To examine this further they used a mouse model of bone tumor–induced pain that closely mimics that seen in human patients, and again found high levels of G-CSF. GM-CSF and their receptors. In vitro studies on nerve tissue from mice showed that G-CSF and GM-CSF made nerves associated with pain (nociceptive nerves) more sensitive. They then found that mice whose paw was injected with G-CSF and GM-CSF withrdrew it more quickly from a painful mechanical or heat stimulus, indicating that they were more sensitive to pain and quickly took action to avoid it, and observed the same in mice with bone tumours.
Having demonstrated a role for G-CSF and GM-CSF in pain they sought to see whether they could block it, and did so by injecting antibodies against G-CSF and GM-CSF in the mouse bone tumour model. But these injections also slowed the growth of the tumours, something that had been observed before, so they wanted to make sure that the lower pain levels were not just due to the tumours being smaller. To do this they injected a viral vector into the nerves adjecent to the tumour that expressed short hairpin RNAs that block the production of the receptors for G-CSF and GM-CSF, which if their theory was correct would stop the signalling peptides from increasing sensitivity to pain. The pain levels were again reduced, even though tumour growth was unaffected, proving that G-CSF and GM-CSF directly increase sensitivity to pain.
This is a discovery that will hopefully allow us to treat cancer pain by local injection of drugs or antibodies that block G-CSF and GM-CSF, something that would help tens of thousands of cancer patients. It also provides an explanation of why some patients who are given GM-CSF and G-CSF to encourage blood cell growth after chemotherapy or before donating stem cells suffer serious bone pain, and may lead to the development of procedures and treatments that might reduce such painful side effects.
Schweizerhof M. et al. “Hematopoietic colony–stimulating factors mediate tumor-nerve interactions and bone cancer pain” Nat Med. published online June 7 2009 DOI:10.1038/nm.1976